A patient comes in with leg pain while walking. Their ABPI test result is borderline, and the duplex ultrasound appointment list is already full for the next three weeks. The question is: what happens to the patient while they wait for the scan?
This is the pressure that vascular departments across the United Kingdom routinely face, not because the clinical pathway is unclear but because the capacity to follow it is not always available. When arterial assessment is delayed, referral decisions stall, and patient outcomes can deteriorate, both clinically and operationally costly.
Our service exists to close that gap. We provide specialist lower limb arterial duplex ultrasound delivered by HCPC/AHCS-registered clinical vascular scientists, working directly alongside your team to maintain diagnostic momentum when in-house capacity is stretched.
Advanced Lower Limb Arterial Duplex Ultrasound UK Services:
Every assessment in our service is conducted by an experienced clinical vascular scientist holding full HCPC/AHCS registration, current CPD compliance, and comprehensive indemnity insurance. These are not optional standards; they are the baseline we require of every scientist working under our service, without exception.
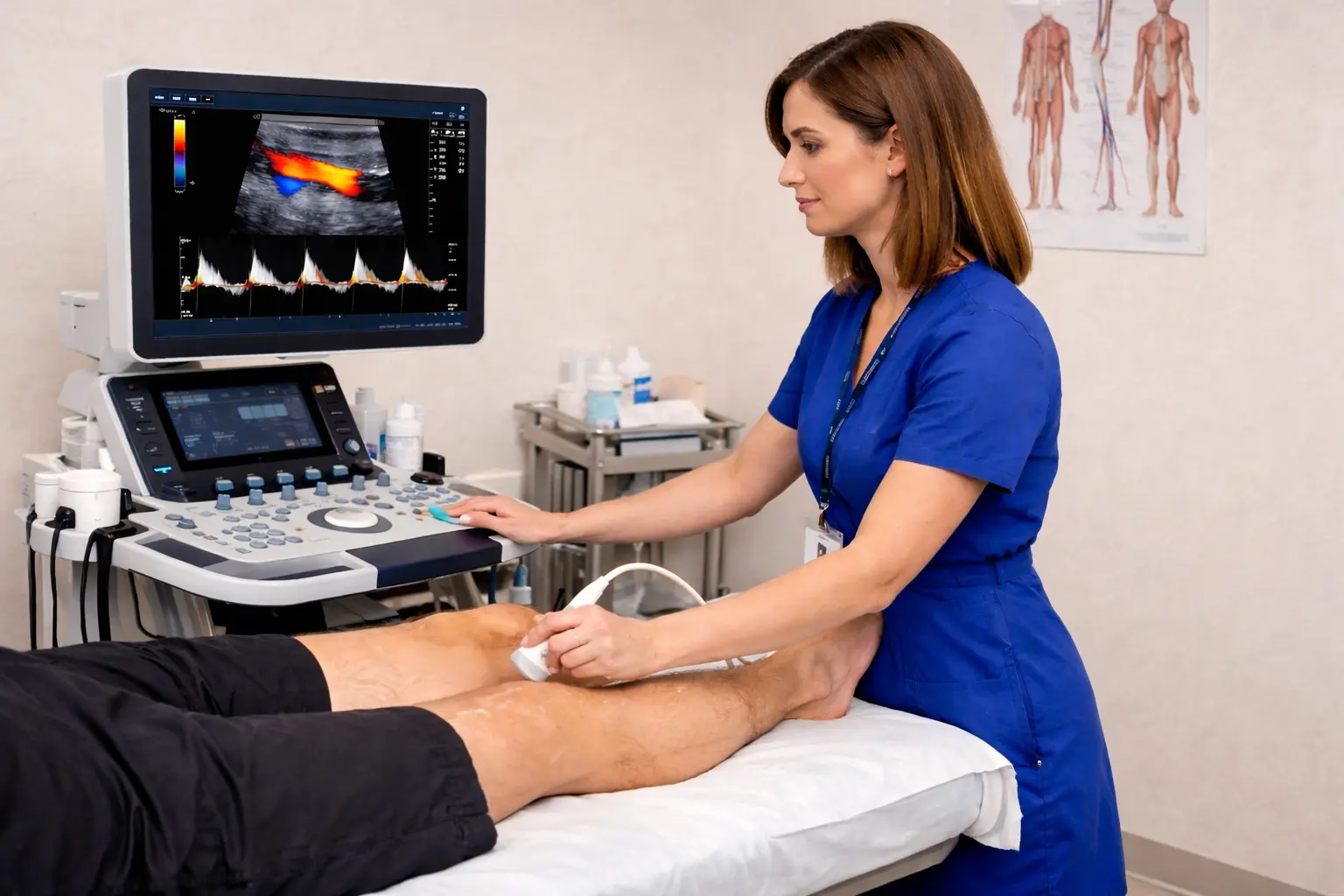
We use state-of-the-art duplex ultrasound equipment calibrated for arterial assessment of the lower limbs. Each leg artery ultrasound scan produces a structured, clinically actionable report designed to support, not replace, your team’s decision-making. The format is consistent across all assessments, which means your clinicians can interpret findings quickly and with confidence regardless of which scientist performed the scan.
The result is a service that functions as a genuine extension of your vascular department: same clinical standards, same reporting rigour, available when your list demands it.
What is a lower limb arterial duplex ultrasound?
- Lower limb arterial duplex ultrasound is a non-invasive vascular imaging technique that combines real-time B-mode imaging of the arterial wall with pulsed-wave Doppler measurement of blood flow velocity. Together, these two modalities allow the examining scientist to identify and characterise arterial stenosis, occlusion, calcification, and collateral flow, providing a level of anatomical and haemodynamic detail that neither modality achieves independently.
- A full lower limb arterial duplex assessment commonly evaluates the femoral, popliteal, and tibial arterial segments, and where clinically appropriate may extend proximally to assess the aorto-iliac circulation, with findings reported by arterial segment and graded by degree of stenosis. This structured approach gives the referring clinician a clear map of the disease distribution, supporting decisions around medical management, angioplasty, or surgical intervention without requiring the patient to undergo more invasive imaging first.
- For vascular teams managing a mixed caseload, from PAD surveillance to pre-operative planning, a duplex ultrasound of the legs remains the first-line imaging modality when revascularisation is being considered, as recommended by NICE and the Vascular Society of Great Britain and Ireland.
What our service delivers for vascular teams:
The practical benefit of an external duplex service is straightforward: it restores diagnostic capacity without the recruitment timeline, on-costs, or long-term commitment of a permanent hire. For departments managing seasonal demand peaks, staff absences, or growing referral volumes, this flexibility has direct implications for waiting time targets and patient flow.
Beyond capacity, the clinical value lies in the quality and consistency of the assessment itself. Each report produced by our scientists follows a standardised format that maps directly to the information a vascular surgeon or interventional radiologist needs at the point of decision. Findings are graded systematically, waveform analysis is documented, and any incidental findings outside the primary referral question are flagged clearly.
For complex cases, patients with calcification affecting ABPI reliability, or those with multilevel disease requiring segmental analysis, our scientists have the experience to adapt the assessment protocol appropriately and annotate the report accordingly, reducing the likelihood of a second scan being required.
ABPI (Ankle Brachial Pressure Index): Initial Screening in UK Vascular Practice:
In the United Kingdom, the ankle brachial pressure index remains the recommended first-line screening investigation for suspected lower limb peripheral arterial disease. The test is quick, non-invasive, and provides a numerical ratio: ankle systolic pressure divided by brachial systolic pressure, which gives the clinician an immediate indication of arterial compromise. An ABPI below 0.9 is generally accepted as diagnostic of PAD; values below 0.5 indicate severe disease requiring urgent assessment.
ABPI serves a gatekeeping function in the diagnostic pathway. By identifying patients with significant arterial compromise at the screening stage, it allows vascular teams to prioritise duplex ultrasound lists appropriately. Directing detailed imaging towards those who will benefit most from it and avoiding unnecessary scans in patients whose index is normal and symptoms have an alternative explanation.
It is worth noting that ABPI has known limitations in patients with heavily calcified vessels, where arterial walls may be incompressible and the index artificially elevated. In these cases. Common in diabetic patients and those with renal disease. Toe brachial pressure index (TBPI) or direct duplex assessment may be more appropriate as the initial investigation. Our scientists are experienced in identifying and documenting these presentations within their reports.
Key Benefits of ABPI Screening:
- Quick and non-invasive assessment of lower limb circulation.
- Identifies patients needing detailed duplex ultrasound scans.
- Supports early detection of peripheral arterial disease.
- Streamlines patient pathways within UK vascular practice.
How Arterial Duplex Ultrasound Works in Practice:
A lower limb arterial duplex assessment begins with a clinical review of the referral information, including symptoms, relevant comorbidities, previous imaging, and the specific clinical question being asked. This context shapes the assessment protocol before the patient is seen, ensuring the scientist examines the most relevant arterial segments in the appropriate sequence.
During the scan, the scientist uses B-mode imaging to visualise the arterial wall, identify plaque morphology, and assess luminal diameter at each segment. Pulsed-wave Doppler is then used to measure flow velocities and characterise waveform patterns. A triphasic waveform indicates normal flow, and a biphasic or monophasic pattern suggests proximal disease. Where velocity ratios across a stenosis exceed established thresholds, the degree of narrowing is graded accordingly.
Once the assessment is complete, findings are compiled into a structured written report, accompanied by representative images from key segments. Reports are typically available within the agreed turnaround window and formatted for direct use in clinical letters, MDT discussions, or referral documentation.
When to request an arterial duplex scan: Clinical indications:
Lower limb arterial duplex ultrasound is appropriate across a range of clinical presentations and pathway stages. The most common referral indications we receive from UK vascular departments include symptomatic PAD with claudication or rest pain requiring disease mapping before intervention; pre-operative assessment for bypass planning; surveillance of existing arterial reconstructions, including bypass grafts and stented segments; assessment of non-healing lower limb ulcers where arterial compromise is suspected; and incidental findings from other imaging that require characterisation.
In departments using ABPI as a screening tool, duplex is typically the logical next step when the index falls below 0.9, when symptoms are disproportionate to the ABPI result, or when the ABPI is unreliable due to vessel calcification. Our scientists are accustomed to receiving referrals at any point in this pathway and will tailor the assessment scope accordingly.
If you are uncertain whether a particular presentation warrants a duplex assessment, our clinical lead is available to discuss referral appropriateness before a formal booking is made. Contact us via the clinical enquiry form.
Recognising peripheral arterial disease: referral triggers for clinical teams
Early referral for duplex assessment is one of the most effective interventions available to vascular teams, yet it depends on PAD being recognised accurately at the point of initial presentation. The clinical features that should prompt consideration of arterial assessment include exertional leg pain that resolves with rest (intermittent claudication), particularly when localised to the calf, thigh, or buttock depending on the level of arterial disease; rest pain in the foot or toes, which indicates critical limb ischaemia and warrants urgent assessment; lower limb ulceration that fails to heal within the expected timeframe, especially in patients with known vascular risk factors; and skin or toenail changes consistent with chronic ischaemia, including hair loss, skin atrophy, and brittle nails.
- Prompt referral at the claudication stage, before disease progresses to critical ischaemia, is associated with significantly better intervention outcomes and lower amputation rates.
- Duplex ultrasound at this stage provides the disease mapping needed to determine whether medical optimisation alone is appropriate or whether revascularisation should be considered.
- Early identification via lower limb arterial duplex ultrasound gives vascular teams the information they need to act decisively rather than managing uncertainty.
How to Detect Arterial Blockages in the Legs Accurately:
Mastering how to detect arterial blockages in the legs is crucial for healthcare centres and scientists aiming to act early. Subtle symptoms and unclear circulation patterns can make early detection challenging. A leg artery ultrasound scan within our reliable vascular duplex ultrasound legs service provides clear visualisation of blood flow, helping identify narrowing or blockages precisely. By using accurate and structured assessments, your team can make confident decisions, prioritise patients effectively, and improve clinical pathways while ensuring timely and informed interventions.
Difference Between Doppler and Duplex Ultrasound:
One of the most common questions we receive from centres new to commissioning external vascular imaging is whether a standard Doppler assessment is sufficient or whether full duplex is required. The distinction matters because the two modalities answer different clinical questions, and selecting the wrong one can result in either incomplete information or unnecessary cost.
| Features | Doppler Ultrasound | Duplex Ultrasound |
| Purpose | Measures the speed and direction of blood flow | Combines flow measurement with visual imaging of artery structure |
| Visual Detail | Limited, primarily audio signals | Detailed image of arterial walls and flow pattern |
| Best For | Quick checks of circulation issues | Comprehensive assessment of blockages, narrowing, or plaque |
| Use in Practice | Detects irregular flow or basic obstruction | Guides precise diagnosis and supports confident decision-making |
| Benefit to Centres | Fast, initial insight | In-depth, reliable information for patients and management |
This clear comparison helps healthcare centres and scientists select the right method, streamlining patient assessment and enhancing the confidence of your vascular evaluations.
Why vascular departments and healthcare centres choose our service:
The decision to commission external vascular imaging involves clinical, operational, and governance considerations. We have structured our service to address each of these directly.
On the clinical side, every scientist we deploy holds full HCPC or AHCS registration, maintains active CPD compliance, and carries comprehensive indemnity insurance. We do not place unregistered or trainee-level scientists into independent reporting roles. The clinical standard is consistent, and the governance trail is clear.
Operationally, we offer flexible engagement models, covering short-term gaps, planned absences, fixed-term contracts, or ongoing sessional support, with availability typically confirmable within 48 hours of initial contact. Reports are delivered within the agreed turnaround window and formatted to integrate directly into your existing clinical documentation workflow.
For centres working towards or maintaining UKAS accreditation or CQC compliance, our service documentation includes scientist credentials, indemnity certificates, and quality assurance records.
We currently support vascular departments and independent treatment centres across the United Kingdom. See the full list of services and coverage areas.
Connect with Us for Seamless Vascular Assessment Support:
Healthcare centres and scientists can access our services easily by completing the form on our website. This simple step allows your team to secure appointments quickly and access structured support for patient care. By connecting with us, you ensure that assessments are scheduled efficiently, reports are delivered promptly, and your centre benefits from reliable, indemnity-backed vascular expertise that strengthens diagnostic confidence and improves patient pathways.
Wrapping up:
Healthcare centres and scientists face increasing pressure to deliver timely and accurate vascular assessments. Early identification of circulation issues in the lower limbs is essential to improving patient pathways and supporting confident clinical decisions. By working with a trusted team of experienced vascular scientists, your centre can access clear, reliable insight that enhances efficiency and strengthens outcomes for every case.
Partnering with a service that offers structured assessments, detailed analysis, and indemnity-backed reporting ensures your team can act quickly and decisively. This collaborative approach not only supports better patient management but also builds long-term trust, allowing your healthcare centre and scientific teams to operate with confidence and clarity in every assessment.
FAQs:
How quickly can centres access your assessments?
Appointment availability is typically confirmed within 24-48 hours of enquiry, depending on location and clinical requirements.
Who performs the assessments, and are they qualified?
All scans are performed by experienced clinical vascular scientists holding HCPC/AHCS registration, maintaining CPD standards, for safe and reliable practice.
Can services support short-term or ongoing needs?
Yes, we offer flexible support tailored to your operational needs, ensuring continuity of service, maintaining efficiency, and avoiding disruption to existing clinical workflows and patient care pathways.
How do reports benefit vascular teams?
Structured, clear, and actionable reports minimise clinical uncertainty, support accurate prioritisation of patients, enhance decision-making, and contribute to improved patient outcomes across vascular assessment pathways.
Why is your service a reliable partner for vascular evaluation?
Our expertise, indemnity-backed assessments, and collaborative approach ensure reliable, transparent, and high-quality results, supporting consistent standards and confident decision-making across UK vascular clinical practice settings.